What I learned later about endometrial ablation is something that still troubles me.
The procedure is performed essentially blind.
As an ultrasound technologist, I have a hard time understanding why imaging guidance isn’t routinely used. Instead of seeing exactly what is being treated, the physician relies on feel and estimation.
Guesswork.
In a procedure meant to permanently alter the lining of the uterus.
To me, it seems so simple to use ultrasound guidance. To visualize the endometrium. To ensure complete and even ablation. To remove uncertainty.
Imaging could take the guesswork out of the equation.
But that isn’t how it was done.
I still had five days left before I could fly home from Thailand.
The medications I received in the emergency room were enough to sustain me while I was there. Enough to dull the pain. Enough to get through each day.
But two days after returning to the United States, I found myself back in an emergency room.
This time, the pain was unbearable.
It felt like contractions.
Deep, intense waves of pain that came and went, leaving me breathless.
What I thought had been a urinary tract infection turned out to be something completely different.
The ablation I had undergone in 2017 had not been successful.
The inferior portion of my endometrium had been fully ablated.
But the upper portion, near the fundus, remained completely intact.
Open.
Still functioning.
Years earlier, after our daughter was born in 2007, I had a tubal ligation.
Because the upper portion of the endometrium was still producing menstrual blood, I was still having periods. But the lower portion of the uterus, which normally allows blood to flow out, had been essentially burned shut.
The blood had nowhere to go.
So my uterus began contracting, trying desperately to expel what it could no longer release naturally.
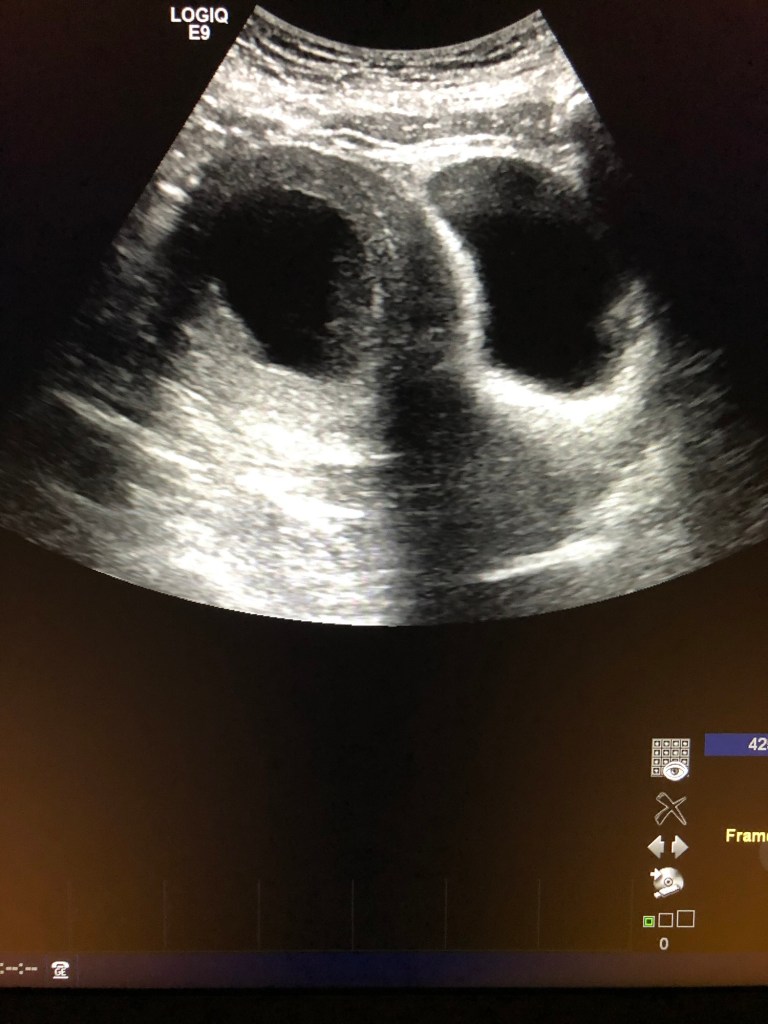
Those contractions were what sent me to the emergency room.
Pain that wasn’t random.
Pain caused by a procedure that was incomplete.
A complication that had been quietly building.
The gynecologist on call that night made the decision to take me into surgery.
I was prepped for an emergency D&C to remove the trapped blood from my uterus.
At that point, there was no other option.
The buildup had become too much. The pain too severe. My body had been trying to do what it could on its own, contracting again and again, but it needed intervention.
The procedure brought immediate relief.
Physically, the pressure was gone.
But emotionally, I was left with even more questions.
How had this happened?
Why wasn’t this a known risk?
Why wasn’t imaging used to ensure the ablation was complete in the first place?
What was meant to be a solution had now led to emergency surgery.
Before taking me to surgery, she came into my room and sat with me. She didn’t rush. She didn’t treat me like just another patient in pain.
She asked if she could pray with me.
Right there in the hospital room, before everything happened, she held my hand and prayed for peace, healing, and strength.
In the middle of fear and uncertainty, that small act meant more than she probably realized.
It was in that moment that I knew I wanted her to be my new gynecologist.
Not just because of her medical care, but because of her humanity.
She saw me.
She comforted me.

Leave a comment